The Dawn of the Internet of Medical Things in 2026
The landscape of medicine has shifted dramatically over the last few years, moving away from the sterile walls of the hospital and onto the wrists and bodies of patients. As a physician witnessing this evolution firsthand, I have seen how the Internet of Medical Things, or IoMT, has transformed the doctor-patient relationship. We are no longer just treating symptoms as they arise; we are monitoring the subtle biological whispers that precede disease.
This connectivity allows for a continuous stream of data that was previously impossible to obtain during a standard fifteen-minute consultation. Devices are now capable of communicating directly with electronic health records, providing a comprehensive view of a patient’s physiology in real-time. This is not science fiction but the current reality of our healthcare ecosystem.
For individuals living with chronic conditions, this constant companionship of technology offers a safety net that significantly reduces anxiety. The integration of sensors into daily life means that a sudden spike in blood pressure or an irregular heart rhythm triggers an immediate alert. It empowers patients to take an active role in their own care, shifting the dynamic from passive recipient to active participant.

Transforming Cardiac Care and Chronic Disease Management
Cardiovascular health remains a primary focus for wearable technology developers, and the precision of these tools has improved remarkably. We are seeing devices that go far beyond simple heart rate tracking to offer medical-grade electrocardiograms and atrial fibrillation detection. This capability is crucial for early intervention, potentially preventing strokes and other severe cardiac events before they occur.
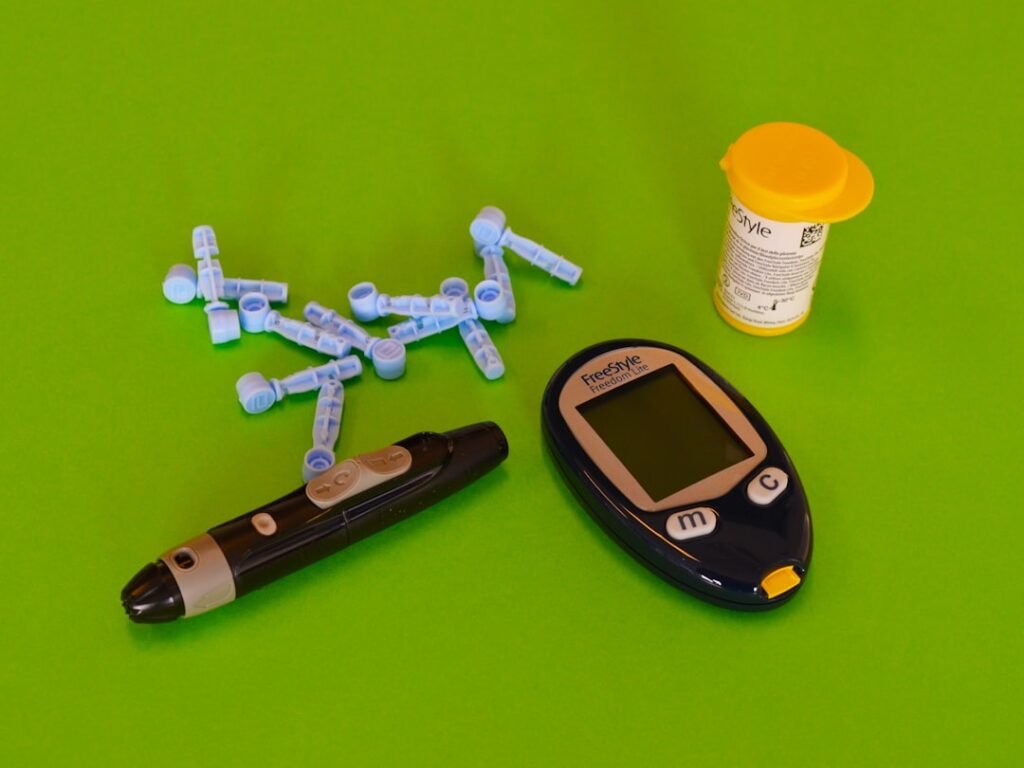
For patients managing diabetes, the synergy between medication and lifestyle monitoring has become a cornerstone of treatment. Recent clinical observations suggest that combining GLP-1 therapies with consistent healthy routines lowers cardiac risks significantly. Wearables play a vital role here by tracking physical activity and glucose trends, providing the data needed to adjust therapies dynamically.
The technology extends to respiratory health as well, with sensors now able to monitor oxygen saturation and respiratory rates with high fidelity. This was particularly relevant during the post-pandemic years, where remote monitoring of respiratory symptoms allowed for safe, home-based recovery. By analyzing these metrics, we can often predict exacerbations in conditions like COPD days before the patient feels a significant decline.
The Power of Predictive Analytics and AI
The true value of wearable technology lies not just in data collection, but in the interpretation of that data through artificial intelligence. Machine learning algorithms can sift through vast amounts of information to identify patterns that are invisible to the human eye. This computational power enables us to move from mere detection to accurate prediction of health events.
By analyzing historical data alongside real-time inputs, these systems can forecast potential health crises. For instance, subtle changes in heart rate variability and skin temperature can signal the onset of an infection or a flare-up of an autoimmune condition. This predictive capability allows physicians to intervene early, prescribing preventive measures rather than reactive treatments.
However, the integration of AI into daily practice requires us to trust the “black box” of algorithmic decision-making. We must ensure that the data feeding these models is high-quality and representative of diverse populations to avoid bias. When used correctly, these tools act as a second pair of eyes, helping to identify the best cardiovascular habits to adopt for long-term wellness based on an individual’s unique physiological profile.
Redefining Access via Telemedicine and Remote Monitoring
Telemedicine has evolved from a convenient alternative to a fundamental pillar of modern healthcare delivery. The ability to monitor patients remotely has dismantled geographical barriers, bringing specialized care to rural and underserved communities. A patient in a remote village can now receive the same level of monitoring as someone living next to a major academic medical center.
This shift is particularly beneficial for our aging population, who may face mobility challenges. With the regulatory landscape adapting to these new realities, we have seen positive changes where the FDA has simplified approval processes for senior-focused health wearables. This ensures that older adults have access to user-friendly devices that keep them safe and connected to their care teams.
The concept of the “hospital at home” is becoming standard practice for stable patients who require monitoring but not intensive care. This approach not only reduces the strain on hospital resources but also protects patients from hospital-acquired infections. It allows for recovery in a familiar, comfortable environment, which has been shown to improve mental well-being and physical outcomes.
Beyond the Wrist: Implants and 3D Printing
While wrist-worn devices are the most visible aspect of this revolution, the technology is rapidly expanding into implants and smart textiles. We are entering an era of 3D-printed medical solutions that are entirely personalized to the patient’s anatomy. From orthopedic implants to bio-printed tissues, the ability to customize treatment materials is changing surgical outcomes.
Innovations in 3D bioprinting are paving the way for the creation of living tissues, such as heart valves and skin grafts, using the patient’s own cells. This reduces the risk of rejection and eliminates the need for lifelong immunosuppressive drugs. It represents the ultimate realization of personalized medicine, where the treatment is literally built from the patient’s own biological blueprint.
Smart clothing is another frontier, integrating sensors directly into fabrics to monitor posture, muscle activity, and vital signs without the need for rigid devices. This is invaluable for rehabilitation and sports medicine, helping individuals in building sustainable physical routines that last without causing injury. These unobtrusive monitors ensure compliance and provide continuous data streams during daily activities.
Navigating Ethics, Privacy, and Health Equity
With the immense benefits of digital health comes the responsibility to manage patient data ethically and securely. The collection of intimate health details raises significant privacy concerns that must be addressed through robust data governance. Patients need to trust that their information is secure and used solely for their benefit, not for commercial exploitation.
There is also the critical issue of the digital divide. We must ensure that the benefits of these advanced technologies are not reserved for the wealthy or tech-savvy. Health equity demands that we design devices that are affordable, accessible, and usable by people of all literacy levels and backgrounds. Programs that incentivize usage can help, such as initiatives where patients can gain benefits for maintaining consistent health tracking.
Ultimately, technology should enhance the human connection in medicine, not replace it. As we integrate these tools, we must remain vigilant against algorithmic bias that could exacerbate existing healthcare disparities. The goal is a healthcare system that is fair, inclusive, and capable of delivering personalized care to every individual, regardless of their socioeconomic status.