For years, CAR-T cell therapy has been hailed as a miracle breakthrough in cancer care—a last-resort treatment that gave new hope to patients with blood cancers like leukemia and lymphoma. But its potential has always faced one daunting wall: solid tumors. Now, with bold advances in research and technology, that wall is beginning to crack. CAR-T is no longer confined to blood—it’s stepping into solid ground.
This evolution in immunotherapy could redefine what’s possible for cancers once considered unresponsive to immune-based strategies. As a health journalist, doctor, molecular researcher, and oncologist, I’ve watched this shift unfold with both scientific skepticism and growing hope. The next frontier of cancer care is here—and it’s changing fast.
What is CAR-T therapy, and why is it revolutionary?
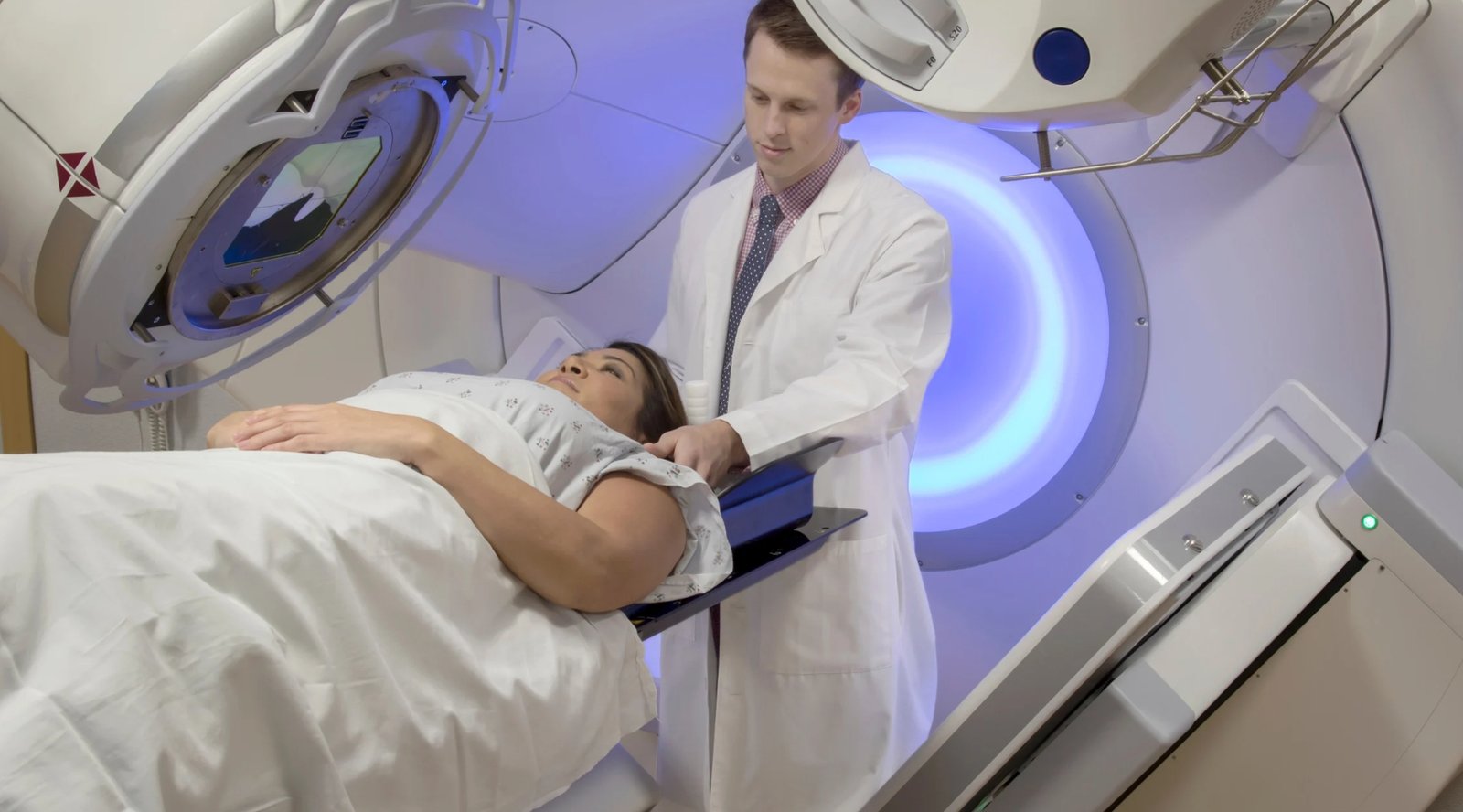
CAR-T stands for chimeric antigen receptor T-cell therapy. It’s a form of personalized medicine where a patient’s own T-cells are collected, genetically engineered to recognize and attack cancer cells, and then reintroduced into the body. In blood cancers, this approach has produced unprecedented remission rates—even in patients who had exhausted all other options.
These engineered cells act like heat-seeking missiles: targeting specific proteins on cancer cells and destroying them with precision. The results, in some cases, have been life-changing. But until recently, this method worked almost exclusively in the liquid realm of blood, bone marrow, and lymphatic tissue.
Why solid tumors are harder to treat
Unlike blood cancers, solid tumors create a protective fortress. Their microenvironment includes dense tissue, immune-blocking proteins, and suppressive signals that make them hard to penetrate. CAR-T cells struggle to survive, expand, and function effectively within this complex terrain.
Additionally, identifying a single antigen target in solid tumors—one that appears on cancer cells but not on healthy ones—is a delicate challenge. Too specific, and the therapy might miss its target. Too broad, and it could harm healthy tissue. These barriers have kept solid tumors largely resistant to CAR-T—until now.
New strategies breaking new ground
Researchers have begun engineering CAR-T cells with added capabilities, often referred to as “armored” CAR-Ts. These enhanced cells may include resistance to immunosuppressive signals or the ability to release supportive cytokines directly in the tumor environment. Some versions are programmed to recognize multiple antigens at once, reducing the risk of tumor escape.
Clinical trials are currently exploring CAR-T applications for notoriously aggressive cancers like glioblastoma, pancreatic adenocarcinoma, and non-small cell lung cancer. Early data suggests these therapies may not produce the same dramatic effects as in blood cancers—yet—but they are extending survival and improving quality of life for patients who previously had few options.
The balance between hope and realism
While the excitement is real, so is the caution. CAR-T therapy remains costly, complex, and—at times—dangerous. It can lead to cytokine release syndrome (CRS) or neurological side effects, particularly if not closely monitored in specialized treatment centers.
Expanding into solid tumors adds new layers of complexity, both scientifically and logistically. Trials remain small, and long-term outcomes are still uncertain. But what once seemed impossible is now inching closer to clinical reality.
What this means for patients
For patients diagnosed with solid tumors—especially those resistant to chemotherapy, radiation, or targeted drugs—CAR-T may soon offer a new path. In the future, treatment plans might include engineered T-cells tailored to a person’s tumor profile, combined with other immunotherapies or precision-guided medications.
This approach represents a shift from fighting cancer with blunt tools to reprogramming the body to do the work itself. It brings us closer to treatments that are both powerful and personal—designed not just to kill cancer cells, but to train the immune system to remember and prevent recurrence.
Looking ahead: the next decade in oncology
CAR-T therapy’s expansion into solid tumors is not a single breakthrough—it’s a process. Each trial, each patient, each engineered tweak builds toward a future where immunotherapy is more adaptable, scalable, and inclusive of diverse cancer types.
Researchers are also exploring off-the-shelf CAR-T products that don’t rely on a patient’s own cells, as well as combination strategies that integrate CAR-T with checkpoint inhibitors, cancer vaccines, or radiation. As these approaches evolve, they will likely reshape how we define survivability in cancer care.
The road from idea to cure is long and filled with complexity. But CAR-T’s emergence into the world of solid tumors marks a powerful turning point. It signals that cancer treatment is becoming smarter, more specific, and—bit by bit—more successful.
For patients, families, and researchers alike, the message is clear: cancer’s survival odds are being rewritten. And the ink is still fresh.

1 Comment
Pingback: Tumor microenvironment drugs: a new way to boost weakened immune systems in seniors - LiveWell Magazine